Apparently Ipsilateral Parkinsonism in a Patient with Chronic Subdural Hematoma
Article information
Abstract
Symptomatic parkinsonism secondary to ipsilateral lesion is rarely reported. Although the contribution of the contralateral lesions was assumed in some cases, the pathomechanism remains undetermined. Herein we report a patient with a subdural hematoma, who developed parkinsonism in the ipsilateral hemibody. Structural and functional imaging suggests the contralateral dopaminergic dysfunction as the major culprit of apparently ipsilateral parkinsonism.
There were a few exceptional cases with hemi-parkinsonism in the ipsilateral side to the lesions [ipsilateral parkinsonism (ILP)] whereas the most patients with secondary parkinsonism had causative lesions in the contralateral hemisphere.1–3 Possible mechanisms for ILP have been discussed but still remain speculative. Herein, we report a patient with ILP. Although the patient had a chronic subdural hematoma (SDH) in the ipsilateral side of parkinsonism, his parkinsonism might be more closely related to hydrocephalus.
Case
A 77-year-old man was admitted for memory loss, clumsiness of the right hand, and gait disturbance. He experienced headache and nausea 4 years before without any history of head trauma, which subsided without specific treatment. His right hand became clumsy around the episode. He had a difficulty in arising from the chair, and began to walk slowly. His symptoms were gradually aggravated afterward.
A neurologic examination showed impaired orientation and memory recall with a 17/30 on Mini-mental status examination. Motor and sensory examination was normal. Deep tendon reflex (DTR) slightly increased in the right knee. His right hand showed a dystonic posture resembling a striatal hand deformity with intermittent resting tremor. Cogwheel rigidity was present in the right arm. He showed a stooped posture and impaired postural reflex. His right leg was less agile with mild external rotation of the foot and with mild shuffling.
Brain MRIs were taken four years before and at admission. Both showed a huge SDH with hydrocephalus without significant interval change. The striatum (STR) was compressed and displaced, more severe on the left side (Figure 1). The compressed thalamus and STR on the right side was displaced downwardly and medially and abutted the right midbrain (MB) (Figure 1A and B, arrows). Dorsal MB lost its convexity with widened ventricle (Figure 1C).
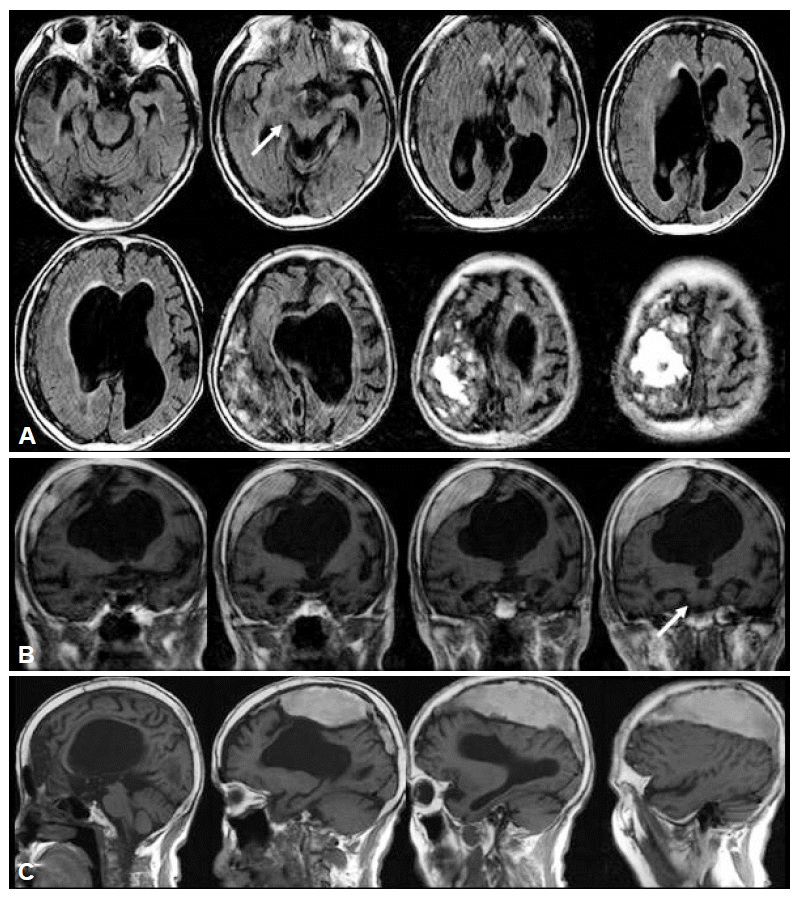
A brain magnetic resonance imaging shows a huge subdural hematoma with calcification over the right cerebral convexity with prominent hydrocephalus (A: axial, B: coronal, C: sagittal). The compressed right brain is displaced abutting the midbrain (arrow), while the left side of midbrain retains its normal contour.
To investigate the nigrostriatal dopaminergic system, positron emission tomography with 18F-fluorinated N-3-fluoropropyl-2-beta-carboxymethoxy-3-beta-(4-iodophenyl) nortropane (18F-FPCIT) was done. 18F-FPCIT uptake was decreased in both STR, more severe on the left side, and similar in both MB. Dopaminergic innervation of the putamen was more decreased in the posterior portion, creating an anterior-to-posterior gradient (Figure 2).
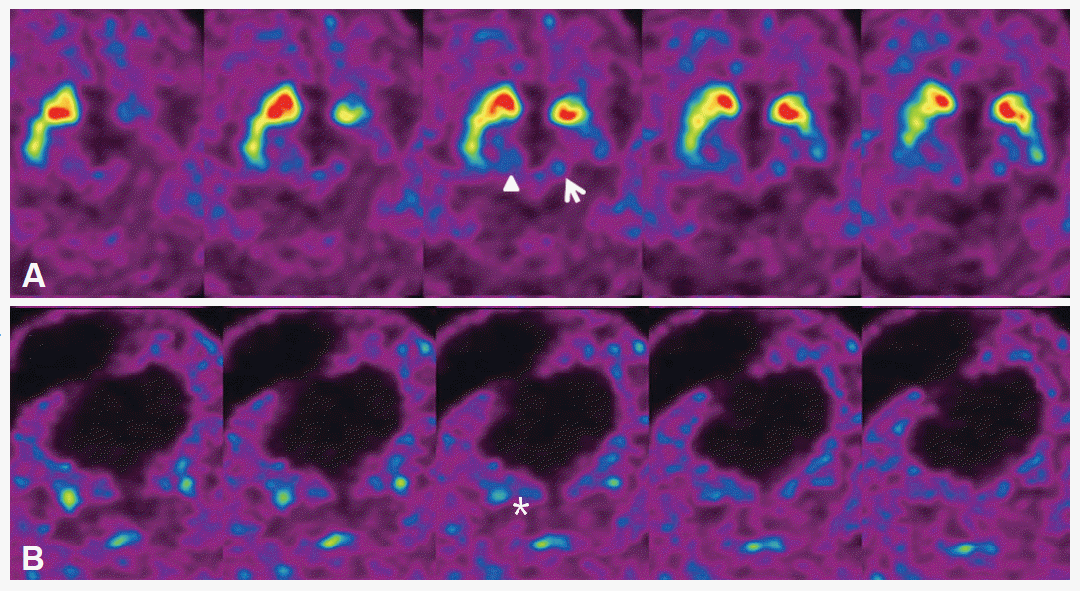
Positron emission tomography with 18F-fluorinated N-3-fluoropropyl-2-beta-carboxymethoxy-3-beta-(4-iodophenyl) nortropane (18F-FPCIT) shows the decreased uptake of 18F-FPCIT in both striatum, which is more severe on the left side (A: axial, B: coronal). In the midbrain, 18F-FPCIT uptake is well preserved on the left side (arrow). The 18F-FPCIT uptake of the right midbrain is preserved but appears as dispersed in the axial image (arrowhead) mixed with that of overlying thalamus (asterisk).
Surgical treatment was waived. His cognitive function was improved with donepezil. Levodopa treatment was mildly effective for his parkinsonism.
Discussion
Subdural hematoma could be hardly considered as the primary diagnosis because of protracted course, slow progression, and the scarce signs of increased intracranial pressure. However, fixed dystonia, increased DTR, and the spastic nature of his gait were suggestive of secondary parkinsonism.
The decreased uptake of 18F-FPCIT in STR could be resulted from direct compression of STR or the disruption of the nigrostriatal pathways.4 As the caudate nuclei retained their convexity, disrupted nigrostriatal pathways may be more likely to be responsible for abnormal 18F-FPCIT uptake. The loss of dorsal convexity of MB would be compatible with the compromised nigrostriatal pathway by hydrocephalus.4 The anterior-to-posterior gradient of dopamine transporter scan could be a feature of pre-synaptic damage.5
In our patient, asymmetric involvement of the contralateral nigrostriatal pathway may result in apparent ILP. It remains enigmatic the absence of parkinsonism in the contralateral side to SDH, in spite of STR abnormality with decreased 18F-FPCIT uptake.