Attention in Parkinson’s Disease Mimicking Suggestion in Psychogenic Movement Disorder
Article information
Abstract
The various reported psychogenic movement disorders (PMDs) include tremor, dystonia, myoclonus, gait disorder, Parkinsonism, tics, and chorea. Although it is not easy to diagnose PMDs, several features such as distractibility, entrainment, suggestion and placebo trial are quite helpful to diagnose. Especially, distractibility or suggestion is a good tool to do in outpatient clinic easily. We describe a patient with parkinsonian features which were improved by internal suggestion to focusing attention. Initially, we suspected her diagnosis as PMDs; however she was confirmed with organic Parkinson’s disease later.
Despite drug therapy, gait disturbance remains a persistent characteristic motor deficit in Parkinson’s disease (PD). External cues, including auditory, visual, or somatosensory, have improved gait in patients with PD.1,2 However, executive dysfunction has also been related to gait difficulty in PD.3 Psychogenic movement disorders (PMDs) are not uncommon in neurological practice and have been reported with variable dyskinesia, including tremor, dystonia, myoclonus, gait disorder, chorea and Parkinsonism. Although the diagnosis of PMD is typically viewed as “diagnosis of exclusion”, some clues, including an abrupt onset, fluctuated symptom, underlying psychiatric comorbidity, or relieving by suggestion, can aid in the diagnosis of PMDs.
Case
This 65-year-old woman had exhibited progressive gait disturbance over a one year period. For 15 years, her son had been in a vegetative state due to head trauma, and she had taken care of him. That had been a source of enormous stress for her. She was diagnosed with depression and had been taking antidepressants for five years. Last year, she felt that her legs dragged and were slow. These symptoms progressed slowly, despite intermittent fluctuation. When she presented in our clinic, she exhibited depressive mood; however, she denied any autonomic symptoms, including postural hypotension, urinary frequency, or constipation.
On neurological examination, she exhibited a mild masked face. Although the speed and amplitude of foot tapping were within normal limits, the amplitude of finger tapping decreased, additionally, speed slowed bilaterally. The motor power of her four extremities showed no weakness and there were no abnormalities on sensory examination. Deep tendon reflex was also normal. During walking, both of her feet dragged and were slowed with a bilateral decrease in arm swing. Sometimes, she hesitated to move exhibiting a glue feature while turning.
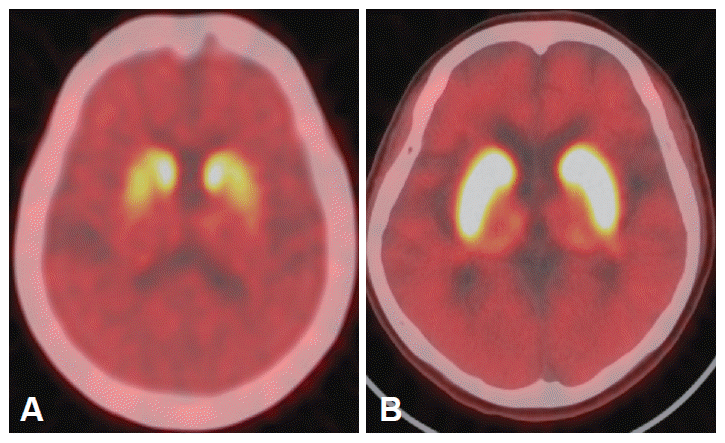
The findings of laboratory studies were unremarkable. A magnetic resonance imaging scan of her brain showed no abnormal findings. Interestingly, the patient reported that she could relieve her symptoms at will. When she concentrated hard on her gait or when she touched her hand to the posterior of her neck, her dragged and slow gait improved dramatically. Also, her abnormal gait improved when the examiner touched his hand to her neck (see video). Based on these curious conditions, we gave her placebo injections along with suggestion. However, there was no symptomatic change following this procedure. Subsequently, she was taken for an Fluoropropyl carbomethoxy-3b-(4-iodophenyltropane) ([18F]-FPCIT) positron emission tomography (PET) scan for evaluation of basal ganglia lesions. Results revealed a reduction in putaminal uptake bilaterally as compared to normal controls (Figure 1). She was then diagnosed with PD, levodopa treatment was initiated. After two months of levodopa treatment, her bradykinesia on both fingers had improved; however, her abnormal gait had not improved markedly. Informed, written consent was obtained after the patient had been given a complete description of the study using a video clip.
Discussion
In this case, when the patient visited our clinic, she had some Parkinsonian symptoms, including masked face, bradykinesia on finger tapping, festinating gait, and glue-like turning. In spite of these common features in PD, the patient’s symptoms fluctuated and she had an underlying psychiatric comorbidity, such as anxiety and depression. Because these findings were common factors for diagnosing of PMDs, we suspected she had PMD. Otherwise, she had been able to relieve her abnormal gait at will or by touching her hand to the posterior neck. These unusual improving features can be found in PMDs rather than in organic disease.4 However, her symptoms did not change following placebo injection, although we found an improvement in her symptom through suggestion-like situations. These findings seemed reasonable in doubtful PMDs. A further, [18F]-FP-CIT PET scan was compatible with PD and furthermore, her symptoms improved after levodopa treatment.
Evidence from some clinical studies has supported the use of cues, including auditory, or somatosensory cues, to improve gait performance in PD.5,6 Executive functions, which has been defined as the ability to plan, manipulate information, initiate and terminate activities, and recognize errors,7 has been shown to play a major role in the gait of PD patient. Attention is an important part of executive function, and in our case, the patient was able to improve her symptoms by focusing her attention. That is, by focusing on gait or touching her hand to the posterior neck during walking, she was able to concentrate and thus, alleviate her symptoms. Furthermore, as with suggestion, her symptom improvement which occurred by touching our hand to her neck during walking caused us to misdiagnose her condition as a PMD, initially. Considering her [18F]-FP-CIT PET scan finding and her response of levodopa, we were able to diagnose her with PD rather than PMD. Although PMDs can mimic the full range of abnormal involuntary movement, including PD, this case made us confuse to diagnose an organic disease, initially, due to dramatic symptomatic improvement by only her attention. We emphasize the importance of attention for improving gait in patients with PD.
Legends to the Video
Segment 1. She had bradykinesia in both hands, which manifested itself in finger tapping which was slowed and fatigued. Bradykinesia was more severe in the hands than the feet.
Segment 2. During walking, she exhibited dragging and slowing gait with decreased arm swing. She also, hesitated to move during turning. These symptoms improved dramatically, when she touched her hand to the posterior of her neck or when the examiner touched his hand to her neck.