Deep Brain Stimulation Battery Exhaustion during the COVID-19 Pandemic: Crisis within a Crisis
Article information
Abstract
Objective
The novel coronavirus disease (COVID-19) pandemic and public health measures to control it have resulted in unique challenges in the management of patients with deep brain stimulation (DBS). We report our experience with the management of acute worsening of symptoms due to battery exhaustion in 3 patients with DBS.
Methods
Patients with DBS for movement disorders who visited the emergency room due to battery exhaustion during the nationwide lockdown from April to May 2020 were included.
Results
Two patients with subthalamic nucleus-DBS for Parkinson’s disease (PD) and one with globus pallidus interna-DBS for generalized dystonia presented with acute worsening of symptoms due to battery exhaustion. Urgent battery replacement was performed in both patients with PD. The patient with generalized dystonia was managed with medication adjustment as he chose to defer battery replacement.
Conclusion
DBS battery replacement can be an emergency. Decisions regarding DBS battery replacement should be individualized during this COVID-19 pandemic.
INTRODUCTION
The ongoing novel coronavirus disease (COVID-19) pandemic has forced several countries to impose lockdown to contain the further spread of infection. In India, the first confirmed case of COVID-19 was reported on 30th January 2020, and nationwide lockdown was imposed on 22nd March 2020, with subsequent extensions in three phases until 31st May 2020. During this period, barring a few exceptions, all modes of transport were restricted, nonessential establishments were shut down, a nationwide curfew was imposed to prevent public gatherings, and social distancing and the use of face masks were advised. The lockdown and prioritization of healthcare services for acute care of COVID-19 may have helped to a certain extent in handling COVID-19. However, it has put patients with chronic illnesses, such as Parkinson’s disease (PD), who need regular follow-up, at a healthcare disadvantage [1-4]. A matter of concern is that most health centers are postponing elective procedures to conserve hospital resources for the management of COVID-19. Even though there was no restriction for healthcare emergencies, elective and routine follow-up appointments were deferred to prevent the spread of COVID-19. Furthermore, apart from the lack of public transportation, which was a deterrent for patients’ to access healthcare, several patients harbored apprehensions about visiting hospitals as they feared the possibility of contracting the infection. The pandemic crisis poses challenges for the management of patients with deep brain stimulation (DBS) for various indications. These patients may face difficulty visiting their doctors for programming and for battery replacement in the case of battery exhaustion, as it may not be considered a healthcare emergency. We report our experience with the management of acute worsening of symptoms due to battery exhaustion in 3 patients with DBS for advanced PD (two) and generalized dystonia (one).
METHODS
This study was conducted at the National Institute of Mental Health and Neurosciences, Bengaluru, India. Patients with DBS for movement disorders who visited the emergency room due to DBS battery exhaustion during the nationwide lockdown from April 2020 to May 2020 were included in this study. A chart review of these cases was performed, and details pertaining to their pre-DBS, pre- and post-DBS battery exhaustion and post battery replacement assessments were analyzed.
RESULTS
Case 1
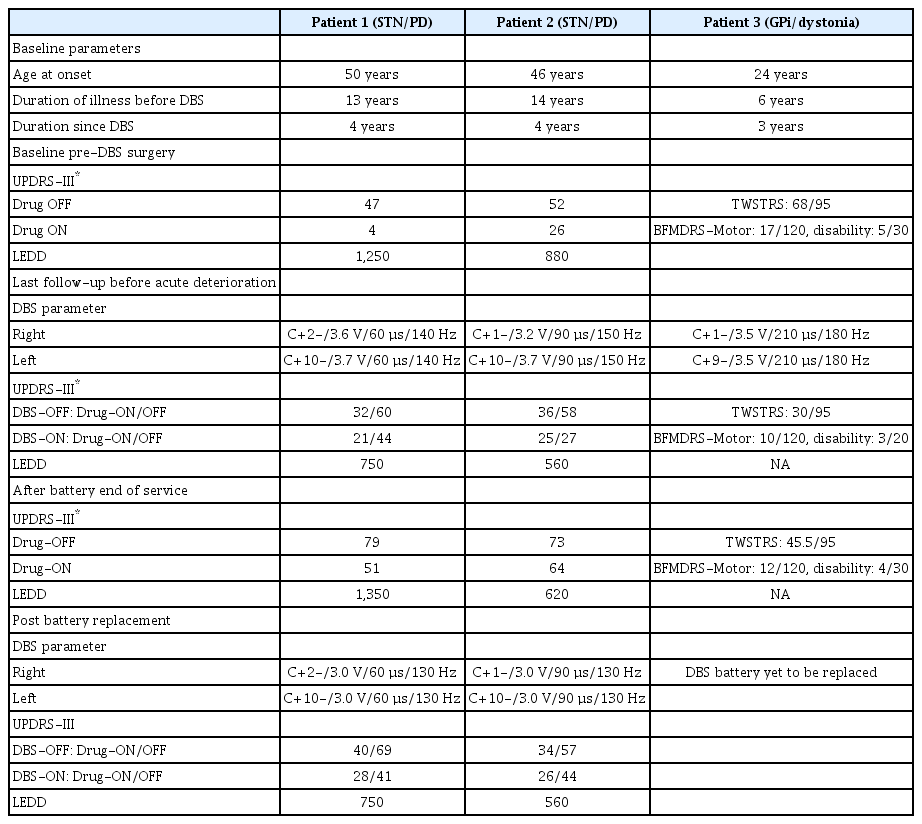
A 67-year-old man with advanced PD of 17 years had undergone subthalamic nucleus DBS (STN-DBS) implantation with a nonrechargeable neurostimulator 4 years ago. He was independent for activities of daily living (ADL) with a modified Rankin scale (mRS) score of 2. He presented with an acute-onset akinetic rigid state of 2 days duration with no fever, seizures, loss of consciousness, or incontinence (Figure 1). He was due for a follow-up 2 months prior to presentation but had deferred due to the COVID-19 pandemic. The patient was conscious, alert, oriented, afebrile, tachycardic, tachypneic and had normal blood pressure and oxygen saturation. He was anarthric with severe asymmetrical parkinsonism and an akinetic rigid state. The rest of his neurological and systemic examination was normal. His Unified PD Rating Scale-III (UPDRS-III) OFF-state score was 79 (Table 1). On evaluation, his DBS battery was found to have reached end-of-service status. The results of routine blood investigations, including serum creatine kinase, were normal. Dopaminergic medications were optimized with mild improvement (UPDRS-III ON-state score 51). Following screening and testing for COVID-19, the patient was taken up for battery replacement under general anesthesia. Significant improvement was noted after battery replacement and the restoration of neurostimulation. At the time of discharge, he was ambulant and independent for ADL with a UPDRS-III (DBS-ON, Drug-ON) score of 28.
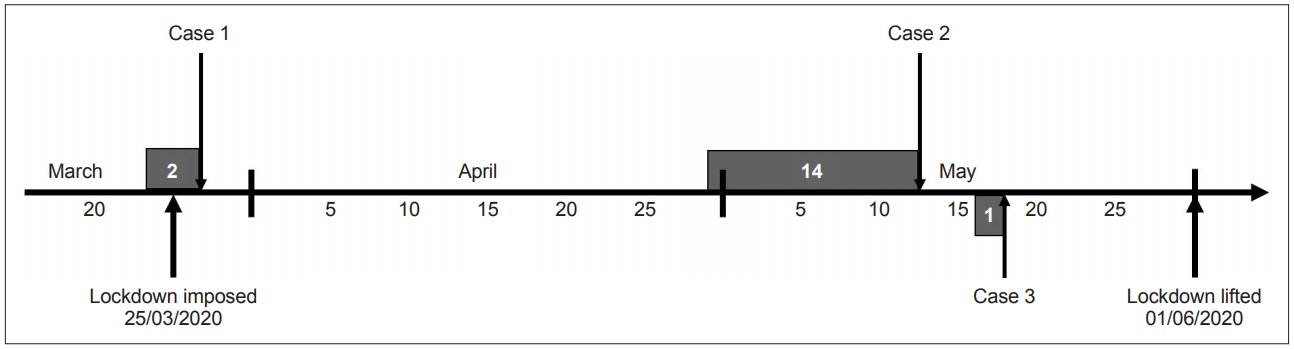
Timeline showing associations between lockdown and patient-related events. Gray boxes indicate days from the onset of the worsening of symptoms to presentation at the emergency room.
Case 2
A 60-year-old woman with advanced PD of 17 years had undergone STN-DBS implantation with a nonrechargeable neurostimulator 4 years ago. Following this, she was independent for ADL with an mRS score of 2. She presented with worsening parkinsonian symptoms for 2 weeks prior to presentation (Figure 1). Owing to the lockdown, she was unable to visit our hospital for evaluation. However, she consulted a nearby neurologist and had her dopaminergic medications adjusted, and she noticed mild improvement. At presentation, the patient was conscious, alert, and oriented. She had asymmetric parkinsonism with a UPDRS-III OFF-state score of 73 (Table 1). The rest of her neurological and systemic examination was normal. On evaluation, her DBS battery was found to have reached end-of-service status. Routine blood investigations, including serum creatine kinase, were normal. Further elevation of the dopaminergic medication dose was attempted; however, there was no significant improvement (UPDRS-III ON-state score 64). Following screening and testing for COVID-19, the patient was taken up for battery replacement under general anesthesia. Significant improvement was noted after battery replacement and the restoration of neurostimulation. At the time of discharge, she was ambulant and independent for ADL with a UPDRS-III (DBS-ON, Drug-ON) score of 26.
Case 3
A 33-year-old man with idiopathic gradually progressive generalized dystonia of 9 years had undergone bilateral globus pallidus interna DBS implantation 3 years prior to the current presentation. Following DBS, he had significant improvement in dystonia (Table 1) and had maintained the improvement at his last follow-up, which was 6 months prior to the emergency presentation. He presented to our emergency room with acute overnight worsening of dystonia, and evaluation revealed end-of-service status of the battery. The patient was advised to undergo a battery replacement; however, owing to financial constraints, he deferred the surgery to a later date. His medication was optimized to improve the current worsening, and he was discharged.
DISCUSSION
The lockdown and restrictions placed to prevent the spread of COVID-19 may have significant implications for both patients with DBS and those scheduled to undergo surgery [5]. Planned DBS surgeries for various indications have been rightly put on hold as they are elective surgeries and hospitals may be burdened with the care of patients with COVID-19. However, over time, elective DBS surgeries will have to be resumed as they cannot be put on hold indefinitely, and most patients are considered for DBS surgeries due to inadequate management with medication. In places where there are no limitations of resources, a proper plan of action in consultation with the DBS team, appropriate health authorities and hospital administration should be formulated to establish a system to prioritize patients and determine extra precautions necessary during hospitalization and surgery to resume elective DBS surgeries. However, surgical intervention is an emergency in patients with battery malfunction due to exhaustion or other device-related issues, such as lead fracture or migration, electrical malfunction or infection. These patients are at risk of developing life-threatening complications of interrupted neurostimulation, such as DBS withdrawal syndrome, acute dystonic crisis, and the return of disabling tremor, which can be refractory to medication.
All 3 cases discussed in this report were scheduled for a routine follow-up a few months prior to the acute worsening; however, they deferred the visit as their conditions were well maintained, and in view of the evolving COVID-19 pandemic, they wanted to reduce the risk of infection. As there was no restriction for healthcare emergencies during lockdown, two of our three cases visited the emergency room shortly after the onset of symptom worsening. Two patients underwent emergency battery replacement as they did not have satisfactory improvement with medication alone. Although it is difficult to accurately predict when exactly the battery may run out, patient-controlled programmers can alert patients to impending end of service through the elective replacement indicator, which appears approximately 4–6 weeks prior to complete discharge of the battery. Patients may notice gradual worsening in symptoms as the battery runs out; however, there can be sudden worsening with complete drainage of the battery. Apart from battery exhaustion, acute worsening may also be due to lead fracture or migration, which could occur secondary to falls or a neck injury.
All patients with DBS who are due for battery replacement should be counseled about the need to check battery status with the patient-controlled programmer and to contact the treating neurologist if the programmer shows the elective replacement indicator or end-of-service status. In PD, long-standing STN-DBS (> 5 years), advanced disease (> 15 years), low-dose dopaminergic medications and older age are risk factors for DBS withdrawal syndrome and should be a high priority for battery replacement in the case of battery exhaustion [6,7]. Urgent battery replacement or troubleshooting hardware malfunction is a high priority in most patients but should be decided on an individual basis after discussing the risk of complications, exposure risk to COVID-19 for both patients and healthcare workers and the availability of resources during the pandemic. If the battery cannot be replaced immediately, patients can be temporarily managed with dose escalation until the battery is replaced. The dose of medication can also be pre-emptively escalated prior to the exhaustion of the battery to compensate for decreasing neurostimulation and to avoid sudden worsening of symptoms, DBS withdrawal syndrome or acute dystonic crisis.
Programming-related follow-ups can be supplemented with video teleconsultations and the use of the patient-controlled programmer. First-time programming in PD can be deferred by asking patients to continue on their presurgery medication dose. For other indications where medications alone would not suffice and for reprogramming in the case of symptom worsening or stimulation-related side effects, video teleconsultation can be offered, and remote programming can be attempted with the help of the patient-controlled programmer. If these measures fail, individual decisions can be made about in-person consultation or medication adjustment after discussing the various risks involved.
DBS surgeries during this pandemic may pose extra challenges and several logistical issues. Testing for COVID-19 in those undergoing surgeries should be decided based on prevailing guidelines issued by regulatory bodies. No emergency procedure should be delayed due to the lack of a COVID-19 test report. There may be an unprecedented increase in the total cost of DBS surgeries during the pandemic due to the inclusion of the cost of testing for COVID-19 and protective equipment to prevent the spread of infection. Difficulty in procuring DBS-related hardware and any additional costs should be discussed with the manufacturer and suppliers, as these devices may need to be imported. These costs may be additional expenses that insurance companies may not be willing to cover.
CONCLUSIONS
The COVID-19 pandemic and subsequent restrictions to control it have resulted in many unprecedented challenges for DBS-related patient management. Although the control of the pandemic is the first priority and of utmost importance, care should be taken to ensure that patients with other illnesses are not sidelined. With no clear end of the pandemic in sight, elective surgeries such as DBS implantation cannot be indefinitely put on hold, and a plan of action is necessary to restart these surgeries. Better use of telemedicine and patient-controlled programmers should also be considered. This pandemic should motivate us to generate better guidelines to address DBS-related issues during such scenarios.
Notes
Conflicts of Interest
The authors have no financial conflicts of interest.
Author Contributions
Conceptualization: Vikram Venkappayya Holla, Ravi Yadav, Pramod Kumar Pal. Data curation: Vikram Venkappayya Holla, Koti Neeraja, Bharath Kumar Surisetti, Shweta Prasad. Supervision: Dwarakanath Srinivas, Pramod Kumar Pal. Writing—original draft: Vikram Venkappayya Holla, Koti Neeraja, Shweta Prasad. Writing—review & editing: Bharath Kumar Surisetti, Nitish Kamble, Dwarakanath Srinivas, Ravi Yadav, Pramod Kumar Pal. Approval of final manuscript: all authors.
Acknowledgements
None.