Psychogenic Balance Disorders: Is It a New Entity of Psychogenic Movement Disorders?
Article information
Abstract
The various reported psychogenic dyskinesias include tremor, dystonia, myoclonus, gait disorder, Parkinsonism, tics, and chorea. It is not easy to diagnose psychogenic movement disorders, especially in patients with underlying organic disease. We describe three patients with balance and/or posture abnormalities that occur when they stand up, start to move, or halt from walking, although their gaits are normal. One had an underlying unilateral frontal lobe lesion. All patients improved dramatically after receiving a placebo-injection or medication. These abnormal features differ from the previously reported features of astasia without abasia and of psychogenic gait disorders, including recumbent gait. We describe and discuss the patients’ unique clinical characteristics.
In the past, the diagnosis of psychogenic movement disorders (PMDs) was one of exclusion. Now, clinicians have accepted that it is a separate entity and have developed some new criteria for the diagnosis, based on patients’ detailed histories and clinical signs.1–3 Despite these efforts, it is not easy to diagnose PMDs, especially in patients with underlying organically caused abnormal movements. Approximately, 10% to 15% of PMD patients have an underlying organic movement disorder as well. Psychogenic gait disorders (PGDs) have variable clinical manifestations, including extremely slowing gait, dystonic gait, bizarre gait, astasia-abasia and buckling of the knee, during walking.4–6 However, there have been no previous reports of patients who have only abnormal balance and/or posture, with normal gait. Here, we present three patients who had curious balance and posture abnormalities and whom we confirmed as suffering from psychogenic disorders.
Case
Case 1
A 58-year-old man visited our clinic with a complaint of unsteady posture. In March 2001, he was found to have an aneurysm in the left anterior communicating artery, and he underwent the clipping procedure for this aneurysm. After surgery, the patient reported a tremulous feeling in the right leg when he was standing, but not when walking or lying. The right leg’s tremulous feeling during standing soon disappeared. However, due to a subsequent syncopal episode, he was given a brain MRI in July 2006. This MRI showed cerebromalacia in the left frontal area and total occlusion in the distal left internal carotid artery (Figure 1A). In February 2007, the patient visited our clinic due to disequilibrium during standing. Although his posture appeared abnormal during standing and turning, he had never fallen while standing or walking. He had no family history of neurological or psychiatric disorders and his past medical history was unremarkable. On examination, his speech was normal and he had no rigidity or bradykinesia. However, he showed all the frontal lobe release signs, including glabellar, snout, and palmo-mental signs. With regard to motor power, he showed mild weakness in the right upper extremity and hypethesia (2/10) on the right side of his body on the touch and pinprick test. Deep tendon reflexes were normal. His routine laboratory results were within normal limits and his brain single photon emission computerized tomography showed decreased blood flow in the left frontal area (Figure 1B). When he stood up from a chair, his posture appeared unsteady; that is, for a while he would experience a bouncing posture, sometimes mixed with an ataxic posture. However, his feet moved forward readily, there was no freezing feature during walking. His stride and stance were also normal during walking, but when he halted, especially while turning, the bouncing and/or ataxic posture would re-appear. On the pull test, his bouncing posture became aggravated but he did not fall down. We performed a placebo test to evaluate the patient for psychogenic disorder. One minute after the placebo was injected, his abnormal bouncing posture diminished a little, and five minutes later, his posture on standing was normal. However, nine minutes after the placebo injection, his abnormal posture re-appeared (Video Segment 1). We suggested that he had a psychogenic balance disorder and referred him to the psychiatric department.
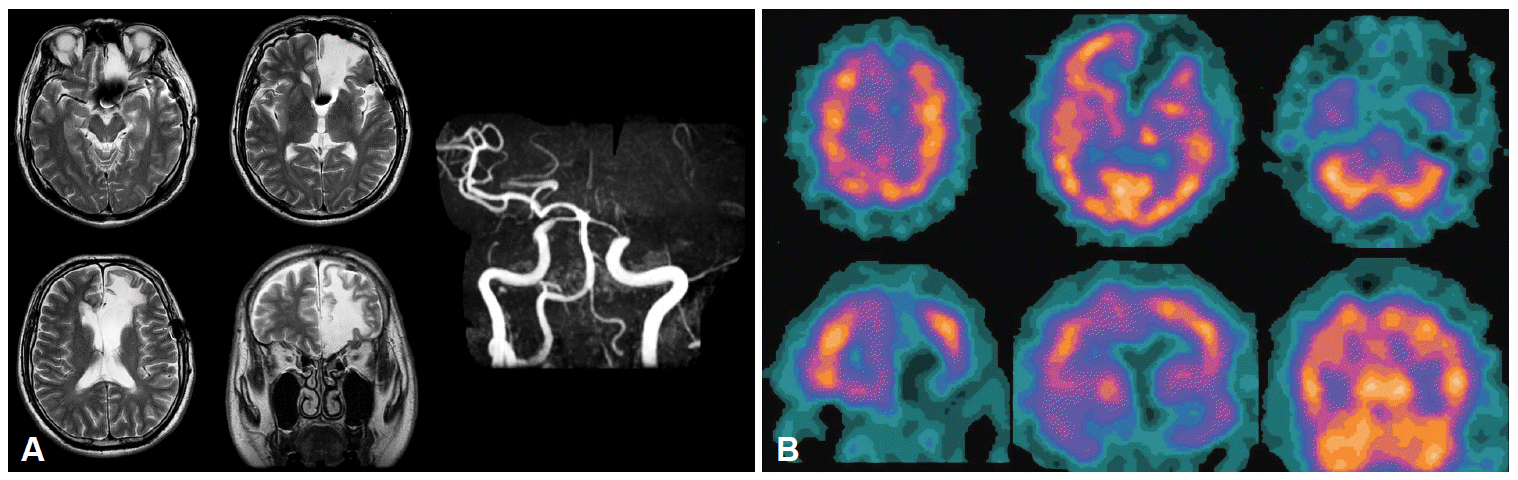
A: The brain MRI and magnetic resonance angiography of Case 1 showed cerebromalacia in the left frontal area and total occlusion at the distal left distal internal carotid artery. B: The brain single photon emission computerized tomography of Case 1 showed decreased blood flow in the left frontal area.
Case 2
A 13-year-old boy visited our clinic because for the past month he had been unable to stand without spreading his legs. One month prior, a friend had struck blow on the patient’s chest area during school. Two hours later, he hyperventilated and suddenly felt chilled, dizzy, and disequilibriated. The day after the injury, a pediatrician at a pediatric epilepsy center evaluated him. The patient’s brain MRI and routine electroencephalography (EEG) were normal. The findings of his routine laboratory tests were within normal limits. His abnormal posture had persisted for one month before he was referred to our clinic. When we first saw him, he could not stand due to swaying and falling backward. His abnormal posture appeared whenever he narrowed his stance to within the width of his shoulders. However, he had no abnormal posture when he stood with his feet spread well beyond shoulder-width. His abnormal posture remained the same regardless of whether his eyes were open or closed. His gait did not appear abnormal regardless of his stance or stride during walking. Our nerve conduction study of his lower extremities was unremarkable. We injected 1 mL of normal saline into the antecubital vein, as a placebo. The patient’s bilateral swaying and backward-falling disappeared completely 5 minutes after this injection, and the effects lasted 10 minutes. Twenty minutes after the injection, his symptoms reappeared (Video Segment 2). We referred him to a psychiatrist and his symptoms were fully improved after psychotherapy.
Case 3
A 51-year-old woman presented with a feeling of falling backward when standing up from her chair, which she had experienced for four days. She reported that recently, she had been feeling anxious, due to experiencing a vivid dream every night. Four days before her clinic visit, she had begun feeling as though someone would pull her back whenever she stood up and started to move forward. Her husband had lost his job two months previously, and her mother, who had suffered from Alzheimer’s disease, had passed away due to a head trauma one month previously. On examination, we discovered no abnormal findings. However, whenever she would stand up from her chair or start to walk from a standing start, she experienced retropulsion. Despite her unsteady posture, she had never fallen while standing or walking (Video Segment 3). Her unsteady posture was unchanged regardless of whether her eyes were open or closed. Routine laboratory test results were unremarkable. Likewise, her brain MRI, routine EEG and neurophysiologic studies, including nerve conduction velocity on both lower extremities and brainstem auditory evoked potential, were all normal. We gave her placebo medication for her anxiety to evaluate her for possible PMD due to an anxiety disorders. After two weeks of medication, her abnormal movement disappeared. She was referred to a psychiatrist and was diagnosed with general anxiety disorders.
We obtained informed, written consent from all patients after they had received a complete description of our intended use of their video clips.
Discussion
All three patients presented here had unusual postures when standing. Despite their unsteady postures, they had never fallen while standing or walking, and all had no nystagmus and postural hypotension. Considering this curious phenomenon, astasia without abasia can be similar with this abnormal feature. “Astasia without abasia” is therefore defined as an inability to keep a stationary position although the legs are under control when walking or assuming and maintaining an upright posture. The most common cause of astasia without abasia is peripheral neuropathy.7 However, our patients presented with some patterns, those differed from classic astasia. We found that some patients had unsteady standing postures during certain of their posture changes: standing up from their chairs, coming to a halt from a walk, or moving forward from a standing start (Case 1 and 3). The patient in Case 2, in particular, experienced a unique symptom; his unsteady posture depended solely on the width of his stance. Although the typical astasia pattern is a known phenomenon among PGDs,4 this atypical form of astasia without abasia has not been reported to date. Boogaarts et al.8 reported a patient with a recumbent gait, which they regarded as a variant of astasia-abasia. Unlike the patient in their study, none of our patients experienced any change in symptoms that depended upon whether the eyes were open or closed.
Typically, most patients with PMD have certain characteristic features, including an abrupt onset, inconsistent, incongruent patterns, simultaneous multiple symptoms, and a previous history of minor injury.2 Our patients had histories that included abrupt onset and incongruent patterns, although Case 1 had an unclear onset of symptoms. Case 1 had a unique underlying brain lesion on the frontal lobe area. Considering that lesion, his bouncing and ataxic features are understandable.9 The core clinical elements of frontal gait disorders can be characterized as hypokinetic, rigid gait with ataxic, impaired postural reflexes, akinetic and a tendency to fall. In general, cerebrovascular disease of the frontal lobe is a main cause of frontal gait.9 Early descriptions of frontal gait syndromes emphasized the ataxic elements, because researchers considered involvement of frontopontocerebellar pathways to be the most likely mechanism.10 In frontal lobe dysfunction, both isolated gait ignition failure and primary progressive freezing gait can be accompanied by normal stepping, once walking is underway, and by preservation of balance and postural reflexes.11,12 Patients with frontal lobe abnormalities commonly present with a combination of the above clinical signs, each of which may vary in severity. However, our patient was likely to complain of fluctuating symptoms and other incongruous neurological deficits, including memory loss and dyscalculia, despite their mental functioning being normal.
Actually, PMD is notoriously difficult to diagnosis. We are accustomed to making use of suggestions, distractions, and/or triggering method to differentiate between organic and psychogenic origin. Although placebos can be used to confirm psychogenic disorders, we have to consider that placebos might affect the trust component of the doctor-patient relationship.13 Fortunately, the placebo affected all of the patients in this study, so we were able to confirm them as having PMD, although one of them had underlying organic abnormalities. Considering the phenomenological aspects of these patients, we might regard them as experiencing a psychogenic balance disorder rather than astasia without abasia of psychogenic origin.
Legend to the Video
Segment 1. A 58-year-old man experiences bouncing and/ or ataxic features upon standing or turning, but these disappear during walking. On the pull test, the bouncing feature becomes aggravated, but the patient does not fall down. After placebo injection, his bouncing posture is slightly diminished one minute later, disappears completely after five minutes, and reappears nine minutes after injection. These dramatic changes correlate with pre-notification the patient received regarding the effects of the injection (Case 1) .
Segment 2. A 13-year-old boy showed that his abnormal posture appears whenever he makes his stance narrower than the width of his shoulders. However, he has no abnormal posture when he stands with his legs spread wide than shoulder-width apart. Bilateral swaying and falling backward disappears completely 5 minutes after placebo injection and the effect lasts for 10 minutes. Twenty minutes after the injection, his symptom appeared again (Case 2).
Segment 3. A 51-year-old woman steps backward several steps, whenever she stands up from her chair or started to walk from a standing start. Two weeks after she begins taking a placebo medication, her abnormal posture during standing up and starting to walk disappears (Case 3).