Parkinsonsim due to a Chronic Subdural Hematoma
Article information
Abstract
Subdural hematoma is a rare cause of parkinsonism. We present the case of a 78-year-old man with right-side dominant parkinsonism about 3 months after a minor head injury. MRI reveals a chronic subdural hematoma on the left side with mildly displaced midline structures. The parkinsonian features were almost completely disappeared after neurosurgical evacuation of the hematoma without any anti-parkinson drug.
The common causes of secondary parkinsonism are drug-induced parkinsonism and parkinsonism-related with structural lesions on the basal ganglia circuits such as brain tumor, infarct or subdural hematoma.1 Generally, onset of parkinsonism in these conditions is relatively clear, acute or subacute course and parkinsonism tend to be reversible after elimination of secondary causes. The pathomechanism of secondary parkinsonism may involve interruption of presynaptic or postsynaptic dopaminergic transmission. Here, we describe a patient with subacute parkinsonism due to a chronic subdural hematoma (CSH) whose parkinsonism was completely disappeared after evacuation of the hematoma.
Case Report
A 78-year-old man noted dysarthria, gait slowness, and clumsiness when using spoon and chopsticks with his right hand for 2 weeks. He had a history of hypertension and experienceed head trauma due to falling down from the bed without altered consciousness about 3 months ago. The patient denied history of any anti-dopaminergic drugs.
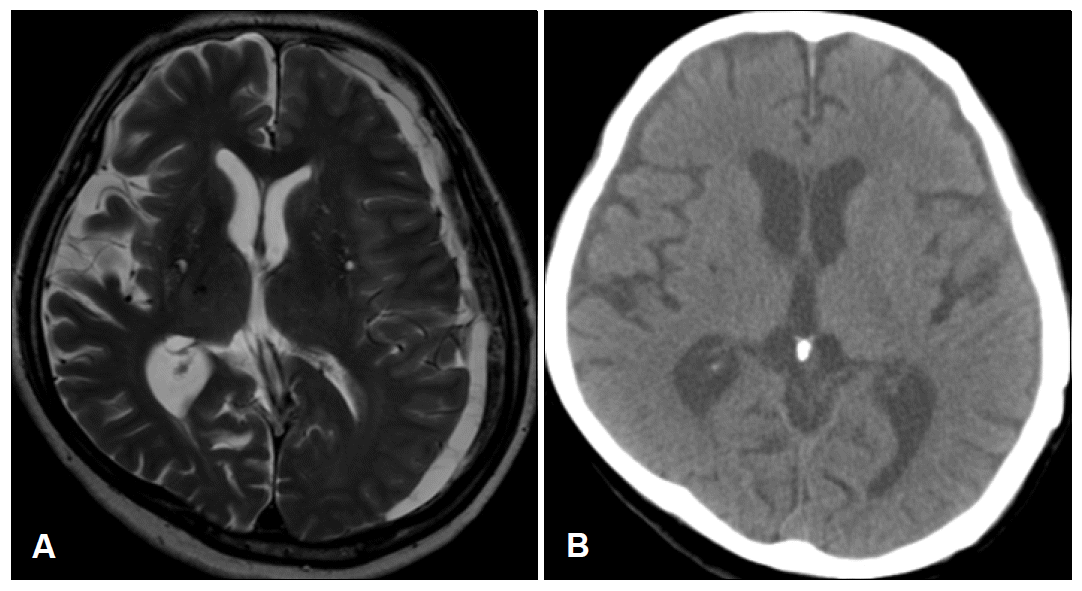
On neurologic examination, mental status was alert and orientation for time and place was impaired. Dyscalculia and impairment in memory registration were noted. Naming, reading, writing and repetition were normal. There were mild hypomimia and rigidity on right extremity. The speed of finger and foot tapping was mildly decreased on right extremities. On gait, there was decreased arm swing on right side with normal base and preserved gait velocity. Neither tremor nor postural instability was shown. There was a slight weakness on right arm showing pronator drift on arm stretching. No other pyramidal sign was checked. Sensory examination was normal. The Unified Parkinson’s Disease Rating Scale (UPDRS) motor score was 27. Brain MRI showed a chronic subdural hematoma in the left convexity with slight midline shift to right (Figure 1A). The hematoma was evacuated by means of burr hole drainage on the next day. After 3 weeks, the rigidity, bradykinesia and gait slowness had almost completely disappeared (UPDRS motor score of 8). The olfactory identification function was normal (Cross-Cultural Smell Identification Test: 9/ in a total of 12). The follow-up brain CT showed no remnant hematoma (Figure 1B).
Discussion
Several cases of parkinsonism related subdural hematomas have been reported. Most were elderly patients with CSH, who subacutely developed parkinsonism. Surgical evacuation2–4 or spontaneous resolution5 of the hematomas induced partial or complete recovery from the parkinsonism. Another case with dopa-responsive parkinsonism after subdural hematoma also have been reported.6 In the latter case, parkinsonian features occurred after surgical treatment of the subdural hematoma. Interestingly, the parkinsonian features occurred ipsilesional side of the subdural hematomas and nigral dopaminergic density using (123I) beta-CIT SPECT scan (DAT scan)6 and [18F] dopa positron-emission tomography7 were markedly decreased on the contralesional striatum of the hematoma, suggesting contralateral nigrostriatal lesion caused by midline shift.
The mechanism leading to parkinsonism in patients with a subdural hematoma is not well understood. It has been suggested that direct compression on the basal ganglia by space-occupying lesions can cause the decreased number of dopaminergic receptors in the striatum which explains parkinsonism secondary to brain tumor.8 Furthermore, the mass effect that compress the midbrain and thus interfere nigro-striatal dopaminergic transmission may also induce parkinsonism. In those mechanism, the levodopa-responsiveness may be depending on the region of compression and the involvement in the midbrain tend to be more responsive rather than basal ganglia compression.9 Alternatively, with a viewpoint that secondary parkinsonisms related with space-occupying lesions are more prevalent in old age, it is possible that space-occupying lesions may unmask underlying subclinical status of Parkinson’s disease in a similar fashion that anti-dopaminergic drugs may unmask preclinical Parkinson’s disease.10 In that smell identification was well preserved in our patient, it is less likely that subdural hematoma may exaggerate preclinical status of PD in our patient.
Although parkinsonism secondary to CSH is rare etiology, it is important to recognize because it is potentially treatable. With careful history taking, it is recommended to take a brain imaging in patients with parkinsonism, especially showing acute or subacute onset.